Facing Health Professional Workforce Challenges in Your Rural Community?
You’re not alone.
Rural communities worldwide are grappling with chronic shortages and high turnover of health professionals (as well as many other skilled workers). This situation is widening the healthcare gap between urban and rural areas. The World Health Organisation identifies workforce maldistribution as a key barrier to equitable healthcare, with rural areas hardest hit, leading to poorer health outcomes.
Traditional strategies, despite decades of effort and significant investment, haven’t solved these challenges. The “rural pipeline” approach, focusing on education and training to boost the supply of rural health professionals, hasn’t effectively addressed the maldistribution problem. It’s clear we need a more impactful solution.
A Fresh Perspective on Rural Health and Social Care
Hi there! We’re thrilled to introduce you to our ground-breaking approach designed to revitalise regional and rural health and social care workforces. The Attract Connect Stay Solution, founded on a decade of Dr. Cath Cosgrave’s research and her acclaimed peer-reviewed Attract Connect Stay Framework, brings an innovative perspective to overcoming health professional workforce challenges in rural areas (it’s also works for other rural industries experiencing skilled worker shortages).

Chronic Workforce Shortages?
On a Recruitment Treadmill?
High Staff
Turnover?
Welcome to the Attract Connect Stay Solution
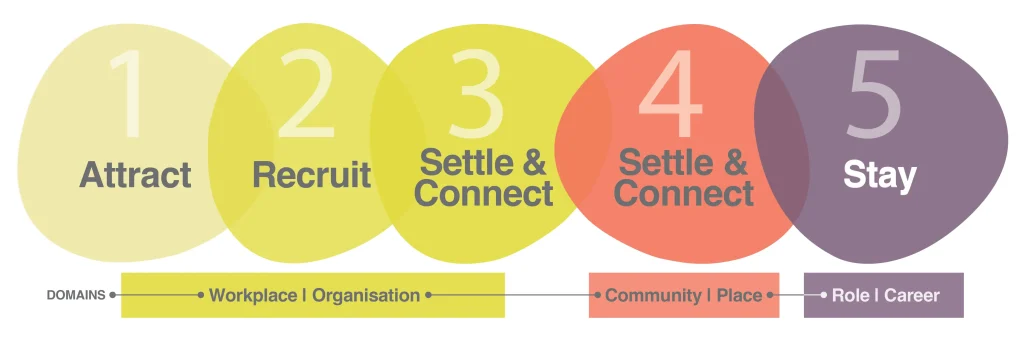
Our Five Implementation Pillars
Our strategy is built on five key pillars, thoughtfully developed to tackle the core issues at the heart of rural skilled workforce dynamics. With a blend of organisational focus and community involvement, we’re setting a new standard for attracting, integrating, and retaining top talent in rural health and social care settings.
Empowering Rural Leaders to Transform Healthcare and Social Care
We empower rural business and community leaders with the tools and insights needed to significantly improve healthcare and social care. Here’s our approach:
- Attract: We guide leaders to identify and engage health professionals who are passionate about rural living, ensuring an ideal fit with the community’s lifestyle.
- Recruit: We share strategies to align recruitment processes with the values and spirit of both the employer and the community, fostering unity and satisfaction.
- Settle & Connect (Organisation): We provide resources to develop comprehensive onboarding programs, making healthcare professionals feel supported, valued, and motivated from day one.
- Settle & Connect (Community): We show how to kickstart your own Community Connector Program. This ensures healthcare staff and their families, along with other skilled workers from outside the region, quickly establish strong local connections, boosting their sense of belonging and long-term commitment.
- Stay: We offer leaders development and retention strategies focusing on personal and professional growth.
Are you maximising your rural health workforce’s potential?
Download this self-assessment checklist to benchmark your organisation against the Attract Connect Stay Framework
A Comprehensive Approach
The Attract Connect Stay Solution goes beyond traditional strategies by covering the entire career lifecycle of rural health professionals. Our goal is to improve healthcare and social care access and outcomes in rural communities, creating a future where every rural area has access to committed health professionals.
Join us in bringing this vision to life.

Establishing the Community Connector Program

Do It Yourself
Self-Paced Online Modules
- 4 x Self-paced Module (Ready, Set, Go, Next)
- 30+ short training videos
- 1 x Course Guide
- 1 x Reflection Workbook
- Toolkit with templates
- Yours to Keep – Downloadable resources and video access

Done Together
With Dr. Cath Cosgrave
- All the Do It Yourself Program plus:
- 3 x 1-hour Ask Me Anything Strategy Calls with Dr Cosgrave
- Anytime online coaching & feedback over 7 weeks
- 7 x weekly 15min Group Coaching Calls
- Bonus: Live Online Community Forum: Q&A with your stakeholders.

Impact Network
With Dr. Cath Cosgrave
- 10 x monthly live webinar and Q&A
- Anytime online coaching & feedback
- Access to ACS 3, 6, 12 month surveys
- Access a tailored CRM for Community Connectors
- 2 x 1-hour Ask Us Anything Strategy Calls with Dr Cosgrave & Bim Rutherford
Master Impactful Recruitment Campaigns
Attract
Good-Fit
Candidates
Staff
Retention
Strategies
Attract Connect Stay - Launchpad Program

Do It Yourself
Self-Paced Online Modules
- 5 x Self-paced Modules covering the ACS pillars
- 20+ short training videos
- 1 x Course Guide
- 1 x Reflection Workbook
- Tool Kit with Templates
- Yours to Keep downloadable resources and video access

Done Together
With Dr. Cath Cosgrave
- All the Do It Yourself Program plus:
- 5 x 1-hour Ask Me Anything Strategy Calls with Dr Cosgrave
- Anytime online coaching & feedback over 10 weeks
- 10 x weekly 15min Group Coaching Calls
- Yours to Keep downloadable resources and video access
- Bonus: Live Online Organisation Forum: Presentation & Q&A with your Board & staff
- Exclusive Workforce Plan

Member Network
With Dr. Cath Cosgrave
- 10 x Monthly live webinar and Q&A
- Anytime online coaching & feedback
- 2 x 1-hour Ask Me Anything Strategy calls with Dr Cosgrave
- Access to ACS 3, 6, 12 month+ surveys
- Access to library of ACS resources
Are you maximising your rural health workforce’s potential?
Download this self-assessment checklist to benchmark your organisation against the Attract Connect Stay Framework
Our Growing List of Clients






















